Figure 7. PT43 presented with Usher syndrome type 2 and two USH2A changes. The molecular diagnosis was confirmed only after follow-up del/dup testing, which revealed a large novel USH2A deletion encompassing exon 27, in trans to a heterozygous USH2A mutation initially detected using NGS-based panel testing. The patient had a clinical phenotype highly suggestive of Usher
syndrome type 2 due to the association of retinitis pigmentosa (RP) with sensorineural hearing loss. A: The fundus photograph (top) demonstrates a waxy nerve pallor, attenuated retinal vessels, peripheral bone spicule deposits,
and nummular RPE loss, typical of RP, presenting on autofluorescence (bottom) as disseminated hypo-autofluorescent fainter
spots and darker, better-defined nummular areas, alongside central hyper-autofluorescence and a faint perifoveal ring of hypo-autofluorescence
(incipient “bull's eye” maculopathy). B: The macular OCT image depicts a mild cystoid macular edema, an epiretinal membrane, thinning of the outer nuclear layer,
and the ellipsoid zone sparing the fovea, also typical of RP. C: Kinetic semi-automated perimetry demonstrates peripheral vision loss with partial preservation of the temporal field in
a pattern consistent with the observed clinical phenotype and the working diagnosis of USH2A-associated Usher syndrome type 2.
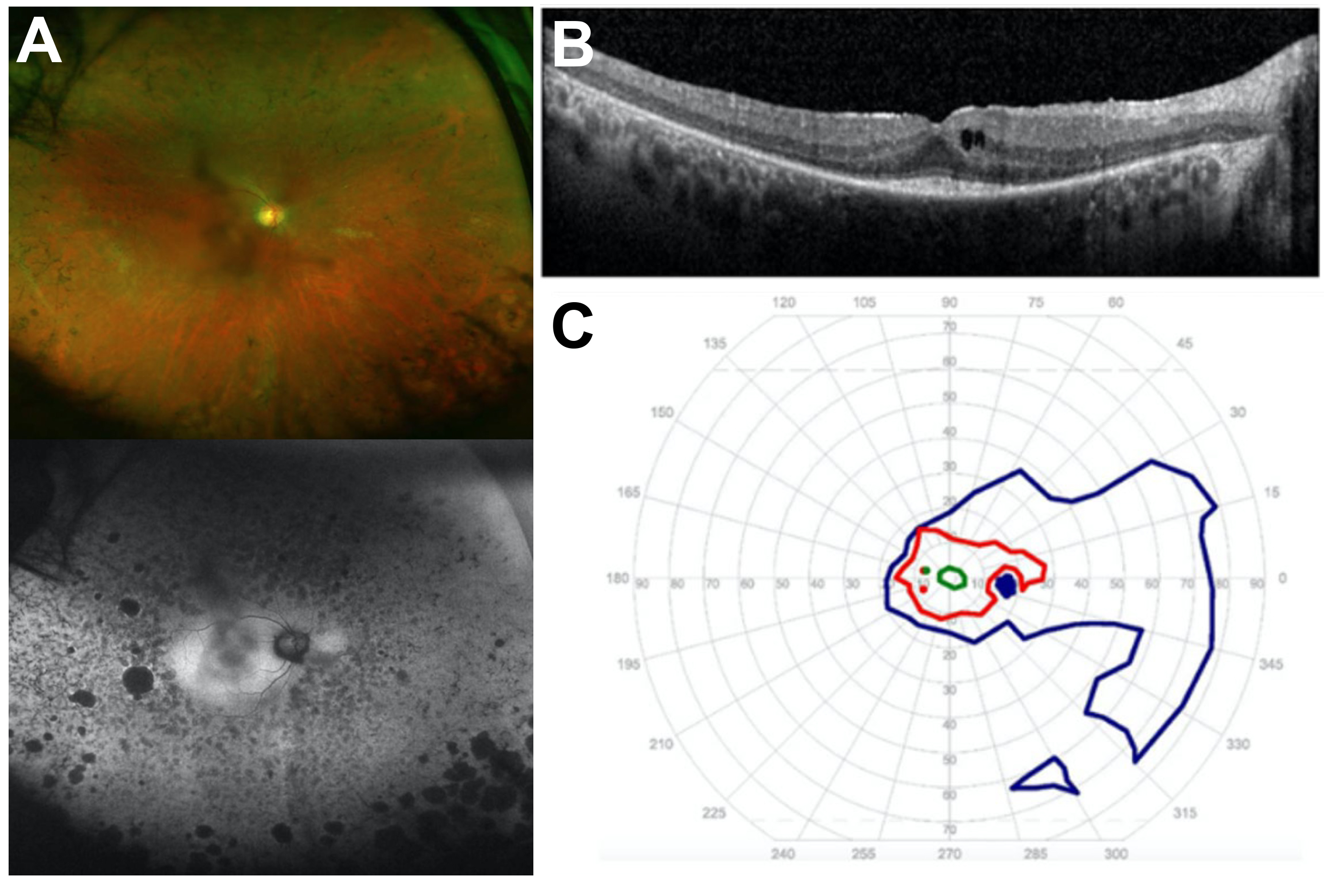
 Figure 7 of
Gupta, Mol Vis 2022; 28:203-219.
Figure 7 of
Gupta, Mol Vis 2022; 28:203-219.  Figure 7 of
Gupta, Mol Vis 2022; 28:203-219.
Figure 7 of
Gupta, Mol Vis 2022; 28:203-219. 