Figure 1. Factors that influence arterial blood pressure. Blood pressure is proportional to cardiac output and the total peripheral
resistance. The latter is dependent on the stiffness of the arterial walls and the level of arteriolar constriction. High
intake of dietary salt causes a rise in extracellular (including plasma) osmolality during the postprandial phases. The elevation
of extracellular osmolality results in an increase in the extracellular fluid (including blood) volume by various mechanisms:
osmotic movement of cellular water to extracellular fluids, stimulation of the thirst center resulting in increased fluid
intake, stimulation of renal salt excretion, and secretion of vasopressin that produces increased renal water retention. All
of these mechanisms reduce the plasma salt level. The blood volume expansion increases cardiac output and induces arteriolar
constriction (to prevent tissue overperfusion); both result in hypertension. The level of arteriolar constriction is regulated
by the activities of vasoconstrictory (stretch, sympathetic activity, angiotensin II, epinephrine, vasopression, endothelin,
etc.) and vasodilatory factors (acetylcholine, NO, etc.). Peripheral resistance increases with age mainly because the resistance
vessels become thicker, stiffer, and narrowed due to arteriosclerosis (the replacement of the medial muscle fibers and intima
by collagen) and atheromatosis (the deposition of lipids in vascular walls resulting in vascular inflammation and endothelial
dysfunction). High salt also increases the blood pressure independent of blood volume expansion by direct effects on arterial
smooth muscles, cardiac myocytes, hypothalamic control of blood pressure, and the local renin-angiotensin system. The blood
pressure–raising effect of dietary salt increases with age mainly because of renal malfunction, which impairs salt excretion,
and vascular alterations, such as arteriolar stiffening and decreased endothelial NO production. In addition, baseline plasma
osmolality increases with age. The scheme shows the transition between an artery and an arteriole that controls tissue perfusion.
In salt-resistant individuals, an increase in plasma osmolality induces a dilation of the artery (which prevents hypertension)
while tissue perfusion remains constant due to arteriolar vasoconstrictory autoregulation. Age-related vessel stiffening impairs
vessel dilation and contributes to the development of salt sensitivity of blood pressure.
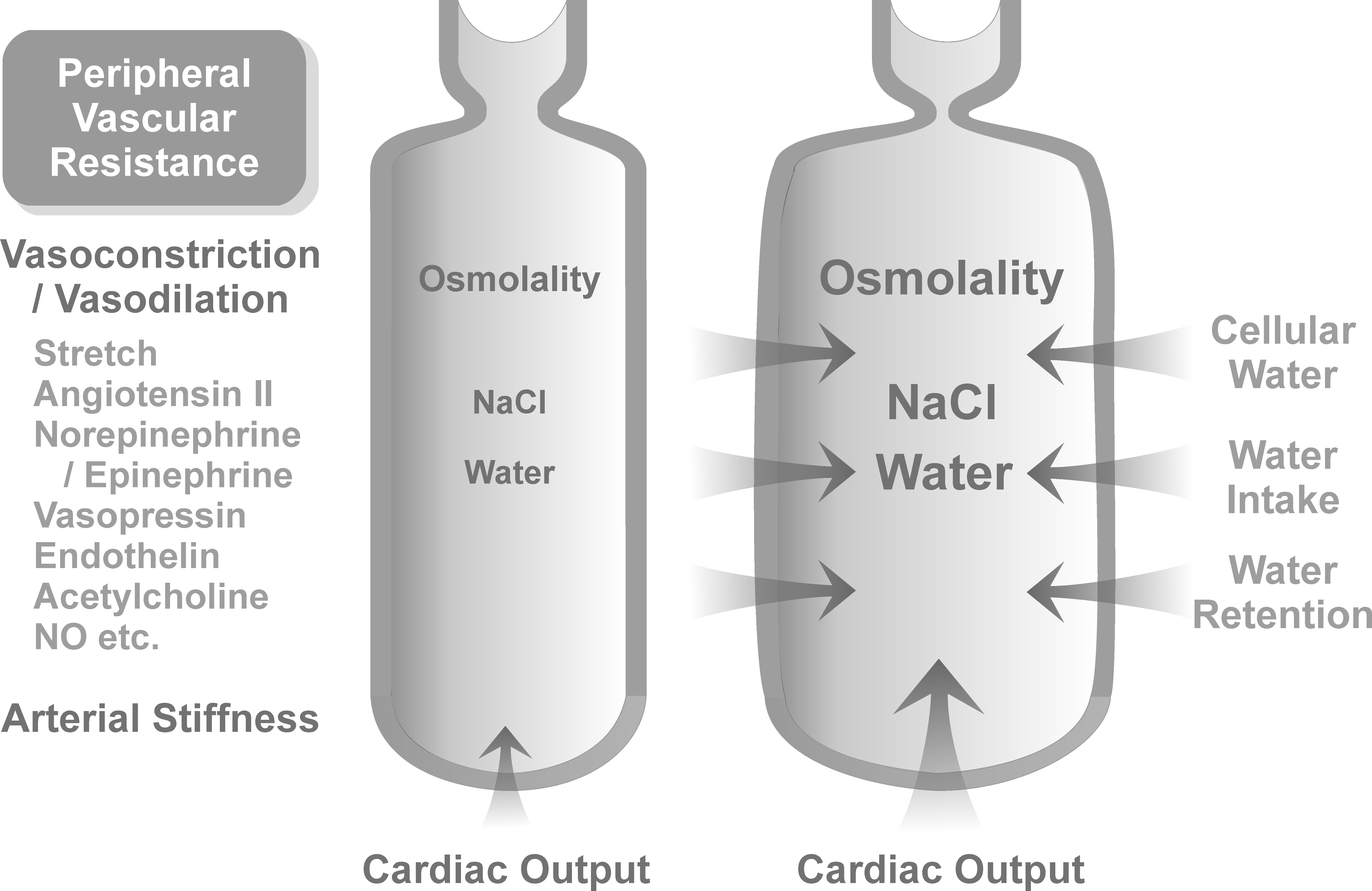
 Figure 1 of
Bringmann, Mol Vis 2016; 22:1437-1454.
Figure 1 of
Bringmann, Mol Vis 2016; 22:1437-1454.  Figure 1 of
Bringmann, Mol Vis 2016; 22:1437-1454.
Figure 1 of
Bringmann, Mol Vis 2016; 22:1437-1454. 